|
Human papillomavirus infection
人乳头瘤病毒感染是人乳头瘤病毒(HPV)的感染。[4]大多数HPV感染不会引起症状并自发消退。[1]在一些人中,HPV感染持续存在并导致疣或癌前病变。[2]癌前病变会增加子宫颈,外阴,阴道,阴茎,肛门,口腔或喉咙癌的风险。[1] [2]几乎所有宫颈癌都是由于HPV有两种类型,HPV16和HPV18,占病例的70%。[1] [6]上述60%至90%的其他癌症也与HPV有关。[6] HPV6和HPV11是生殖器疣和喉乳头状瘤病的常见原因。[1]
HPV感染是由人乳头瘤病毒引起的,这是一种来自乳头瘤病毒家族的DNA病毒,其中已知有170多种类型。[7]超过40种类型通过性接触传播并感染肛门和生殖器。[3]持续HPV感染的危险因素包括第一次性交的早期年龄,多个伴侣,吸烟和免疫功能差[1]。 HPV通常通过持续的皮肤直接接触传播,阴道和肛交是最常见的方法。[3]有时候,它会在怀孕期间从母亲传染给她的孩子。[8]它不会通过马桶座等普通物品传播。[8]人们可能会感染多种类型的HPV。[8] HPV只影响人类。[4] [9]
HPV疫苗可以预防最常见的感染类型。[3]为了最有效,它们应该在感染发生之前使用,因此建议在9到13岁之间使用。[1]宫颈癌筛查,例如Papanicolaou试验(pap)或在使用醋酸后观察子宫颈,可以检测可能发展成癌症的早期癌症或异常细胞。[1]这允许早期治疗,从而产生更好的结果。[1]筛查减少了发达国家宫颈癌的死亡人数和死亡率。[10]疣可以通过冷冻去除。[4]
HPV是全球最常见的性传播感染。[4]大多数人在他们生命的某个阶段受到感染。[3] 2012年,全世界约有528,000例新发病例和266,000例宫颈癌死亡。[11]其中约85%发生在发展中国家。[1]在美国,每年约有27,000例由HPV引起的癌症。[8]大约1%的性活跃成年人患有生殖器疣。[8]虽然自古希腊时代就已经描述过疣病,但直到1907年才发现它们的病毒性质。[12]
目录:
1 症状和体征
1.1 疣
1.2 癌症
1.3 免疫功能低下的个体
2 原因
2.1 传输
2.2 病毒学
3 诊断
3.1 宫颈检查
3.2 口试
3.3 测试男性
3.4 其他测试
4 防治
4.1 疫苗
4.2 避孕套
4.3 消毒
5 治疗
6 流行病学
6.1 美国
7 历史记录
8 研究
9 参考
视频: ↓ 人乳头瘤病毒复制和细胞周期功能障碍
https://cache.tv.qq.com/qqplayerout.swf?vid=y0723uqqne7
视频: ↓ 关于HPV的动画
https://cache.tv.qq.com/qqplayerout.swf?vid=g07238isizb
迹象和症状
Notable HPV[13] types and associated diseases
![Notable HPV[13] types and associated diseases Notable HPV[13] types and associated diseases](data/attachment/forum/201807/16/095207ml8le88f0xs11y7z.png)
值得注意的HPV [13]类型和相关疾病
已经确定了超过170种HPV,它们由数字指定。[7] [14]
一些HPV类型,例如HPV-5,可能会在个体的一生中产生持续存在的感染,而不会出现任何临床症状。 1型和2型HPV可引起一些感染者的常见疣。[引证需要] 6型和11型HPV可引起生殖器疣和喉乳头状瘤病。[1] HPV类型16,18,31,33,35,39,45,51,52,56,58,59,68,73和82被认为是致癌的。[15]
该表列出了HPV感染和HPV相关菌株的常见症状:
Papilloma
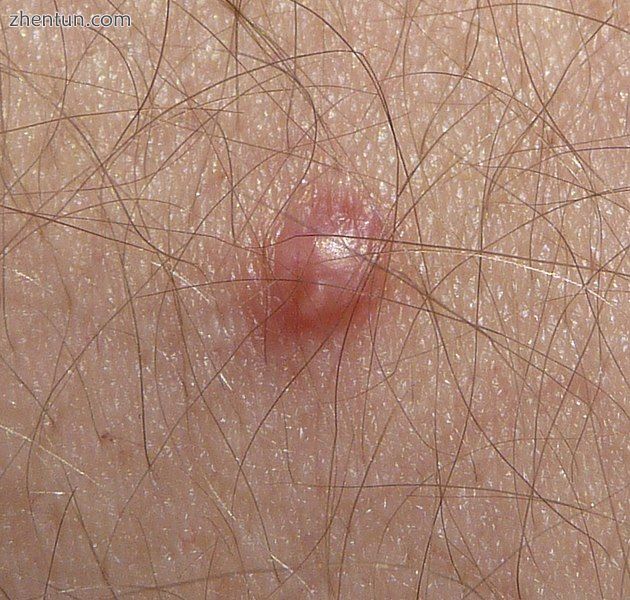
乳头状瘤
A sample DNA test report for HPV Genotype from a laboratory
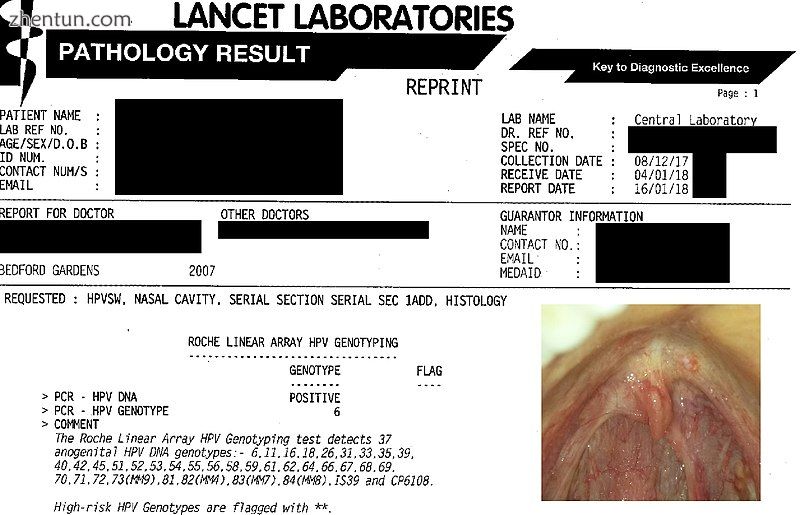
来自实验室的HPV基因型样本DNA测试报告
HPV皮肤感染(“皮肤感染”)非常普遍。[19] HPV皮肤感染可引起非癌皮肤生长,称为疣(疣)。疣是由皮肤外层细胞的快速生长引起的。[20]虽然自古希腊时期以来就已经描述了疣的病例,但直到1907年才知道它们的病毒原因。[12]
皮肤疣在儿童期最常见,通常在数周至数月内自发出现并消退。大约10%的成年人也患有反复发作的皮肤疣。[引证需要]所有HPV被认为能够在皮肤中存在的少量干细胞中建立长期的“潜伏”感染。尽管这些潜伏感染可能永远不会被完全根除,但是认为免疫控制可以阻止诸如疣之类的症状的出现。免疫控制是HPV类型特异性的,这意味着个体可能对一种HPV类型产生抗性,同时仍然对其他类型易感。在一项研究中,在患有疣的人中发现了2型,27型和57型HPV感染,而在皮肤临床正常的人中发现HPV 1,2,33和27型感染[21]。
疣的类型包括:
常见的疣通常存在于手和脚上,但也可能发生在其他区域,如肘部或膝盖。常见的疣具有特征性的花椰菜样表面,并且通常略微凸起在周围皮肤上方。皮肤HPV类型可引起生殖器疣,但与癌症的发展无关。
脚掌上有足底疣;它们向内生长,一般在走路时会引起疼痛。
指甲(甲下),指甲周围或角质层(甲周)下形成甲下或甲周疣。它们比其他地方的疣更难治疗。[22]
扁平疣最常见于手臂,面部或前额。像普通疣一样,扁平疣最常发生在儿童和青少年身上。在免疫功能正常的人群中,扁平疣与癌症的发展无关。[23]
生殖器疣具有很强的传染性,而普通疣,扁平疣和跖疣不太可能在人与人之间传播。
生殖器疣
生殖器区皮肤的HPV感染是全世界最常见的性传播感染。[11]这种感染与生殖器或肛门疣(医学上称为尖锐湿疣或性病疣)有关,这些疣是生殖器HPV感染最容易识别的迹象。
可引起生殖器疣的HPV菌株通常不同于在身体的其他部位引起疣的那些,例如手或脚,或甚至大腿内侧。各种HPV类型可引起生殖器疣,但6型和11型共占所有病例的约90%。[24] [25]然而,总共有超过40种类型的HPV通过性接触传播,并且可以感染肛门和生殖器的皮肤。[3]这种感染可能会导致生殖器疣,尽管它们也可能保持无症状。
绝大多数生殖器HPV感染从未引起任何明显症状,并且在几个月内被免疫系统清除。此外,人们可能会将病毒传播给他人,即使他们没有表现出明显的感染症状。大多数人在生命中的某些时候感染了生殖器HPV感染,目前大约有10%的女性感染了。[11]生殖器HPV感染发生率的大幅增加发生在个体开始从事性活动的年龄。与皮肤HPV一样,生殖器HPV的免疫力被认为是特异性HPV株。
喉乳头状瘤病
除生殖器疣外,HPV 6型和11型感染还可引起喉返性乳头状瘤病的罕见病症,其中喉部[26]或呼吸道其他区域形成疣。[27] [28] 这些疣可能经常复发,可能会干扰呼吸,在极少数情况下会发展成癌症。 由于这些原因,可能需要反复手术切除疣。[27] [29]
癌症
HPV-induced cancers
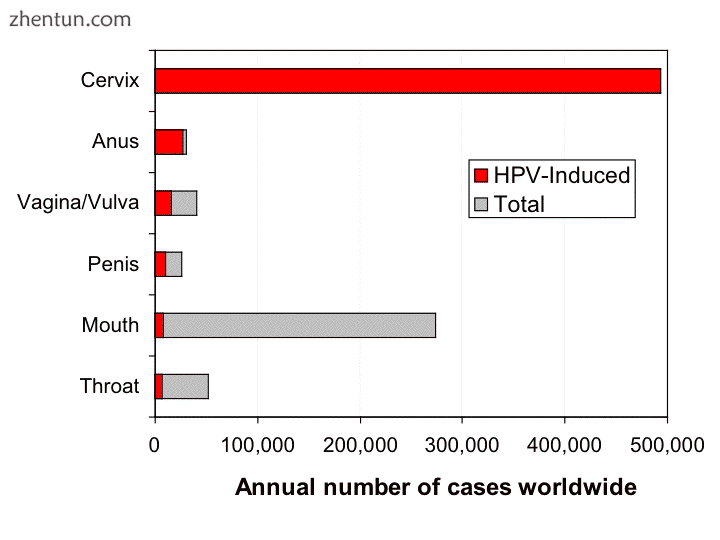
HPV诱发的癌症[30]
大约十几种HPV类型(包括16,18,31和45型)被称为“高风险”类型,因为持续性感染与癌症如口咽癌,喉癌,外阴癌,阴道癌,子宫颈癌,阴茎癌等有关。和肛门。[31] [32]这些癌症通常涉及HPV向分层上皮组织的性传播感染。[1] [2] [30]感染HPV和HIV的个体患宫颈癌或肛门癌的风险增加。[31]
据估计,2002年全球新发癌症病例561,200例(占所有新癌症的5.2%)归因于HPV,使HPV成为最重要的癌症感染原因之一。[30] HPV相关癌症占全球诊断癌症病例总数的5%以上,而且发病率较高的发病率国家每年估计会导致近50万例病例。[30]
在美国,每年约有27,000例由HPV引起的癌症。[8]
美国2004 - 2008年期间HPV相关癌症的数量。[33]
Genome organization of human papillomavirus type 16, one of the subtypes known to cause cervical can ...
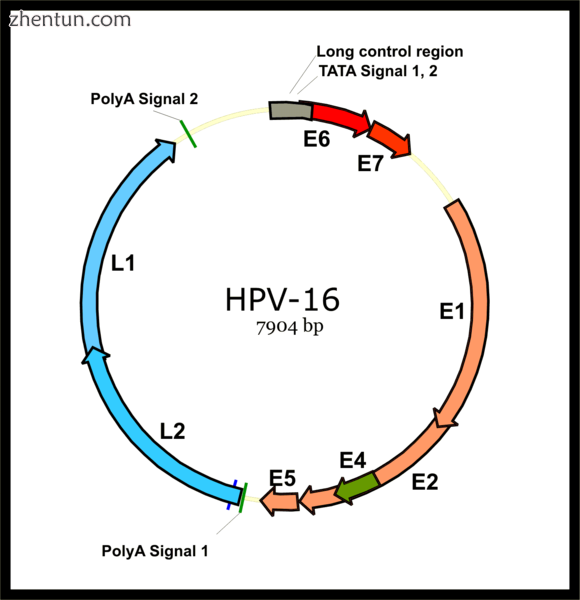
人类乳头瘤病毒16型的基因组组织,已知会导致宫颈癌的亚型之一(E1-E7早期基因,L1-L2晚期基因:衣壳)
在一些受感染的个体中,他们的免疫系统可能无法控制HPV。持续感染高风险HPV类型,如16,18,31和45型,可能有助于癌症的发展。[34]香烟烟雾等辅助因素也会增加这类HPV相关癌症的风险。[35] [36]
人们认为HPV通过整合到DNA和非整合的附加体中而导致癌症。[37]由HPV病毒携带的一些“早期基因”,例如基因E6和E7,充当促进肿瘤生长和恶性转化的癌基因。此外,HPV可通过整合到宿主基因组中诱导致瘤过程,这与DNA拷贝数的改变有关。[38]
E6产生一种蛋白质(也称为E6),可与宿主细胞中称为p53的蛋白质结合并使其失活。通常,p53的作用是阻止细胞生长,并在DNA损伤的情况下促进细胞死亡。 p53还上调p21蛋白,其阻断细胞周期蛋白D / Cdk4复合物的形成,从而阻止RB的磷酸化,进而通过阻止E2F的活化来阻止细胞周期进程。简而言之,p53是一种肿瘤抑制蛋白,它可以阻止细胞周期,并在发生DNA损伤时阻止细胞生长和存活。因此,E6对p53的失活可以促进不受调节的细胞分裂,细胞生长和细胞存活,癌症的特征。
E6还与细胞蛋白E6相关蛋白(E6-AP)有密切关系,后者参与泛素连接酶途径,这是一种降解蛋白质的系统。 E6-AP将泛素与p53蛋白结合,从而标记其蛋白酶体降解。
研究还表明,各种HPV类型与皮肤鳞状细胞癌之间存在联系。 在这种情况下,体外研究表明HPV病毒的E6蛋白可能抑制紫外线诱导的细胞凋亡。[39]
宫颈癌
Cervical cancer caused by HPV.
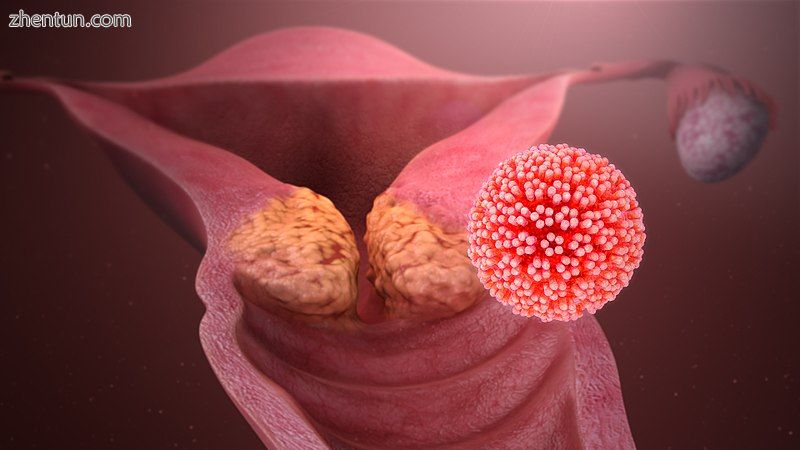
HPV引起的宫颈癌。
几乎所有宫颈癌病例都与HPV感染有关,其中有两种类型,HPV16和HPV18,在70%的病例中存在。[1] [6] [40] [41] [42] [43]
HPV16型是最恶性的菌株,占所有宫颈癌的41%-54%,[40] [44]和许多阴道/外阴癌,[45]阴茎癌,肛门癌和头部癌症和颈部。[46]
2012年,全世界约有528,000例新发病例和266,000例因宫颈癌死亡。[11]其中约85%发生在发展中国家。[1]
大多数宫颈HPV感染被免疫系统迅速清除,并且不会发展成宫颈癌。由于将正常宫颈细胞转化为癌细胞的过程缓慢,因此癌症发生在长期感染HPV的人群中,通常超过十年或更长时间(持续感染)。[27] [47]
非欧洲(NE)HPV16变异体比欧洲(E)HPV16变体显着更致癌。[48]
生殖器癌症
研究表明HPV感染与阴茎和肛门癌之间存在联系。性传播的HPVs在很大比例的肛门癌中被发现。[30]此外,男同性恋和双性恋男性患肛门癌的风险比异性恋男性高17至31倍[49] [50] - 尽管一项调查未发现男男性接触者的HPV感染率与男性之间存在差异。那些只与女性发生性关系的人。[51]
肛门癌的肛门子宫颈抹片检查可能会使一些从事肛交的男性或女性亚群受益。[52]但是,没有达成共识,这种筛查是有益的,或谁应该进行肛门巴氏涂片检查。[53] [54]
头颈部癌症
另见:HPV介导的口咽癌
高风险致癌HPV类型(包括HPV 16和HPV 18)与越来越多的头颈癌相关[42]。
性传播形式的HPV约占口腔和上咽喉癌(口咽癌)的25%。[30]后者通常存在于扁桃体区域,HPV与非吸烟者口腔癌的增加有关[55] [56]。与HPV感染的伴侣进行肛交或口交可能会增加患上这些类型癌症的风险。[57]已经发现口服感染了几种类型的HPV,特别是16型,与HPV阳性口咽癌有关,这是一种头颈癌。[57] [58]该协会不依赖于烟草和酒精使用。[58]在美国,预计HPV将取代烟草作为口腔癌的主要致病因子,预计到2020年新诊断的HPV相关头颈癌的数量将超过宫颈癌病例。[59] [ 60]
近年来,美国经历了由HPV 16型引起的咽喉癌病例数增加。据估计,与HPV相关的喉癌从1988年的每10万人0.8例增加到2004年的每10万人2.6例。 [61]研究人员通过增加口交来解释这些最新数据。此外,研究结果表明,这种类型的癌症在男性中比在女性中更为普遍,需要进一步探索。[62]目前,两种免疫接种Gardasil和Cervarix被推荐给女孩预防HPV相关的宫颈癌,但不是预防HPV相关的喉癌。[63]
已经报道了HPV阳性和HPV阴性头颈癌的突变谱,进一步证明它们是根本上不同的疾病。[64]
肺癌
一些证据表明HPV与上呼吸道的良性和恶性肿瘤有关。国际癌症研究机构发现,与未患肺癌的人相比,肺癌患者患HPV抗体的几种风险更高。[65]在1,633名肺癌患者和2,729名无肺病患者中寻找HPV的研究人员发现,肺癌患者的HPV类型比非癌症患者更多,而在肺癌患者中,患有8种类型的严重HPV的可能性显着增加[66]。此外,通过免疫组织化学和体外研究表达HPV结构蛋白表明HPV存在于支气管癌及其前驱病变中。[67]另一项研究检测了EBC中的HPV,支气管和肿瘤肺组织,并发现受非小细胞肺癌影响的受试者中有16.4%存在HPV感染,但没有一种对照。[68]报告的欧洲和美洲肺癌HPV平均频率分别为17%和15%,亚洲肺癌样本中HPV平均数为35.7%,某些国家和地区之间存在相当大的异质性[69]。
免疫功能低下的人
在极少数情况下,HPV可能会导致免疫系统功能减弱的个体发生疣状表皮发育不良。这种病毒不受免疫系统的影响,导致皮肤细胞过度生成角蛋白,导致类似疣或皮肤角的病变。[70]
原因
性传播HPV分为两类:低风险和高风险。低风险HPV会在生殖器上或周围引起疣。 6型和11型引起90%的生殖器疣和复发性呼吸道乳头状瘤病,在空气通道中引起良性肿瘤。高风险HPV导致癌症,并且由大约十二种确定的类型组成。 16型和18型是造成大多数HPV引起的癌症的原因。这些高危HPV导致世界上5%的癌症。在美国,高危HPVs导致女性癌症病例占3%,男性占2%。[71]
传输
持续性生殖器HPV感染的风险因素包括第一次性交的早期年龄,多个伴侣,吸烟和免疫抑制。[1]生殖器HPV通常通过持续的直接皮肤接触传播,阴道和肛交是最常见的方法,尽管可能发生口交传播。[3] [31]在怀孕期间偶尔会有母亲传染给她的宝宝。它不会通过马桶座等普通物品传播。[8]传染期仍然未知,但可能至少只要可见病变持续存在。即使在病变得到治疗且不再可见或存在后,HPV仍可能传播。[72]
围产期
虽然生殖器HPV类型可以在出生时从母亲传染给孩子,但新生儿中出现的生殖器HPV相关疾病很少见。然而,缺乏外观并不排除无症状的潜伏感染,因为病毒已被证明能够隐藏数十年。 HPV 6型和11型的围产期传播可导致青少年复发性呼吸道乳头状瘤病(JORRP)的发展。 JORRP非常罕见,在美国每10万名儿童中约有2例。[27]虽然如果妇女在分娩时出现生殖器疣,JORRP率会大幅提高,但JORRP在这种情况下的风险仍低于1%。
生殖器感染
由于特定HPV类型的宫颈和女性生殖器感染与宫颈癌高度相关,因此这些类型的HPV感染受到科学研究的大部分关注。
该地区的HPV感染主要通过性活动传播。[73]
在120种已知的人类乳头状瘤病毒中,51种和3种亚型感染生殖器粘膜。[74] 15个被列为高风险类型(16,18,31,33,35,39,45,51,52,56,58,59,68,73和82),三个可能是高风险类型(26, 53和66)和12为低风险(6,11,40,42,43,44,54,61,70,72,81和CP6108)。[75]
如果一名妇女每年至少有一名不同的伴侣,那么她在大学期间接受HPV感染的概率大于85%。[76]安全套不能完全防止病毒感染,因为生殖器周围的区域(包括大腿内侧区域)没有被覆盖,因此会将这些区域暴露给感染者的皮肤。[76]
手
研究表明HPV在同一个人和性伴侣的手和生殖器之间传播。赫尔南德斯每隔一个月测试25个异性恋夫妇中每个人的生殖器和优势手,平均为七个月。她找到了两对情侣,男人的生殖器感染了女性手上的高风险HPV,其中两只手感染了他的生殖器,一只手上的生殖器感染了他的手,另外两只手感染了自己的手,她感染了自己的手。 [77] [78]在这25对夫妇中,手不是传播的主要来源,但它们很重要。
帕特里奇报告说,男性的指尖对高风险HPV的阳性率超过其生殖器的一半(每2年26%)(48%)。[79] Winer报道,14%来自性活跃女性的指尖样本均为阳性。[80]
非性接触手似乎在HPV传播中几乎没有作用。 Winer在她的指尖研究开始时发现所有来自处女女性的14个指尖样本均为阴性。[80]在另一份关于生殖器HPV感染的报告中,1%没有性接触的处女妇女(1 76人)检测出HPV阳性,10%报告非穿透性接触的处女妇女为阳性(72人中有7人)。[81] ]
共享对象
分享可能受污染的物体,例如剃须刀,[72]可能传播HPV。[82] [83] [84]虽然可能,但通过性交以外的途径传播对女性生殖器HPV感染的影响较小。[73]手指 - 生殖器接触是一种可能的传播方式,但不太可能成为重要的来源。[80] [85]
血液
虽然传统上认为HPV不能通过血液传播 - 因为它被认为只感染皮肤和粘膜组织 - 最近的研究称这个概念受到质疑。从历史上看,已在宫颈癌患者的血液中检测到HPV DNA。[86] 2005年,一个研究小组报告说,在57例有垂直或输血感染艾滋病毒感染的性行为儿童患者的冷冻血样中,8例(14.0%)这些样本的HPV-16检测呈阳性[87]。这似乎表明HPV可能通过输血传播。然而,由于通过其他方式进行HPV的非性传播并不罕见,因此无法明确证实这一点。 2009年,一个小组测试了来自180名健康男性供体的HPV澳大利亚红十字会血液样本,随后在15份(8.3%)样本中发现了一种或多种病毒的DNA。[88]然而,重要的是要注意检测血液中HPV DNA的存在与检测血液中的病毒本身不同,并且病毒本身是否能够或确实存在于受感染个体的血液中仍然是未知的。因此,仍有待确定HPV是否能通过血液传播。[86]这是值得关注的,因为目前尚未对HPV进行献血,至少一些组织如美国红十字会和其他红十字会目前似乎不允许HPV阳性个体献血。[89]
手术
已经记录了HPV的医院传播,尤其是外科医生的传播。外科医生,包括泌尿科医生和/或房间中的任何人,在电灼或激光消融尖锐湿疣(疣)期间,通过吸入有毒病毒颗粒而受到HPV感染。[90]有一例激光外科医生在为颅生殖器尖锐湿疣患者提供激光消融术后发生广泛的喉乳头状瘤病。[90]
病毒学
Human papillomavirus infection
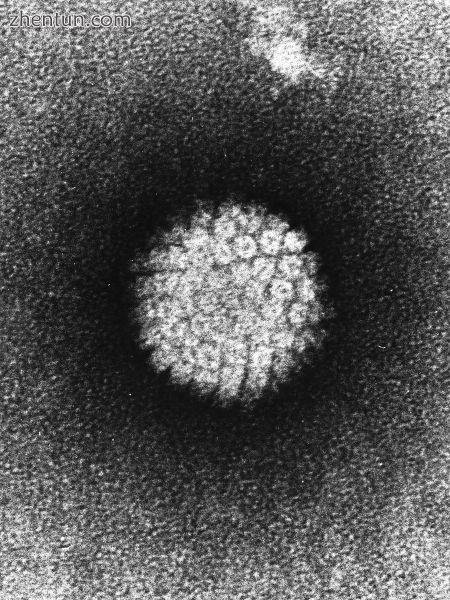
人乳头瘤病毒感染
HPV感染局限于分层上皮的基底细胞,这是它们复制的唯一组织。[91]病毒不能与活组织结合;相反,它通过微观磨损或暴露基底膜片段的其他上皮创伤感染上皮组织。[91]感染过程缓慢,开始转录需要12-24小时。据信,所涉及的抗体起着主要的中和作用,而病毒粒子仍然存在于基底膜和细胞表面。[91]
HPV病变被认为是由感染的基底角质形成细胞的增殖引起的。感染通常发生在宿主中的基底细胞通过扰乱的上皮屏障暴露于感染性病毒时,如在性交期间或在轻微的皮肤擦伤之后发生的。 HPV感染尚未显示为溶细胞性;相反,病毒颗粒由于脱皮细胞的退化而释放。 HPV可以在没有宿主的情况下存活数月和低温;因此,患有足底疣的人可以通过赤脚行走来传播病毒。[25]
HPV是一种小型双链环状DNA病毒,基因组大约有8000个碱基对。[31] [92] HPV生命周期严格遵循宿主角质形成细胞的分化程序。据认为,HPV病毒粒子通过微擦伤感染上皮组织,其中病毒粒子与推定的受体如α整合素,层粘连蛋白和膜联蛋白A2结合[93],通过网格蛋白介导的内吞作用导致病毒粒子进入基底上皮细胞。和/或小窝蛋白介导的内吞作用取决于HPV的类型。[94]此时,病毒基因组通过未知机制转运至细胞核,并以每个细胞10-200个病毒基因组的拷贝数建立自身。然后发生复杂的转录级联,因为宿主角质形成细胞开始分裂并且在上皮的上层中变得越来越分化。
各种HPV毒株的系统发育通常反映了智人的迁移模式,并表明HPV可能与人群一起多样化。研究表明,HPV沿着反映人类宿主种族的五个主要分支进化,并与人口一起多样化。[95]研究人员已经确定了HPV16的两种主要变种,欧洲(HPV16-E)和非欧洲(HPV16-NE)。[96]
E6 / E7蛋白
高风险HPV类型的两种主要癌蛋白是E6和E7。 “E”表示这两种蛋白质在HPV生命周期的早期表达,而“L”表示晚期表达。[42] HPV基因组由六个早期(E1,E2,E4,E5,E6和E7)开放阅读框(ORF),两个晚期(L1和L2)ORF和一个非编码长控制区(LCR)组成。 。[97]在宿主细胞被感染后,病毒早期启动子被激活,并且含有所有六个早期ORF的多顺反子初级RNA被转录。然后,这种多顺反子RNA经历活性RNA剪接以产生多种mRNA同种型。[98]其中一个剪接的同种型RNA,即E6 * I,可作为翻译E7蛋白的E7 mRNA。[99]然而,病毒早期转录受试者病毒E2调节和高E2水平抑制转录。 HPV基因组通过破坏E2 ORF而整合到宿主基因组中,从而阻止E6和E7上的E2抑制。因此,病毒基因组整合到宿主DNA基因组中增加E6和E7表达以促进细胞增殖和恶性肿瘤的机会。表达E6和E7的程度与最终可能发展的宫颈病变的类型相关。[92]
在癌症中的作用
E6 / E7蛋白使两种肿瘤抑制蛋白p53(由E6灭活)和pRb(由E7灭活)灭活。[14]认为病毒癌基因E6和E7 [100]改变细胞周期,以使分化的宿主角质形成细胞保持在有利于病毒基因组复制扩增和随后的晚期基因表达的状态。与具有泛素连接酶活性的宿主E6相关蛋白结合的E6起到泛素化p53的作用,导致其蛋白酶体降解。 E7(在致癌HPV中)充当初级转化蛋白。 E7竞争视网膜母细胞瘤蛋白(pRb)结合,释放转录因子E2F以反式激活其靶标,从而推动细胞周期前进。所有HPV均可诱导瞬时增殖,但只有菌株16和18可在体外永生化细胞系。还显示HPV16和18不能单独使原代大鼠细胞永生化;需要激活ras致癌基因。在宿主上皮的上层中,晚期基因L1和L2被转录/翻译并用作包裹扩增的病毒基因组的结构蛋白。一旦基因组被衣壳化,衣壳似乎经历氧化还原依赖性组装/成熟事件,其与跨越基底上和角质化上皮组织层的天然氧化还原梯度相关联。这种组装/成熟事件可以稳定病毒粒子,增加它们的特异感染性。[101]然后,病毒体可以在宿主上皮的死角中脱落,病毒生命周期仍在继续。[102] 2010年的一项研究发现,E6和E7参与了HPV诱导的癌症中β-连环蛋白的核积累和Wnt信号传导的激活[103]。
延迟期
一旦HPV病毒体侵入细胞,就会发生活动性感染,并且可以传播病毒。在鳞状上皮内病变(SIL)发展并且可以临床检测之前可能经过几个月到几年。从活动性感染到临床可检测疾病的时间可能使流行病学家很难确定哪个伴侣是感染源。[104]
净空
大多数人在没有医疗行动或后果的情况下清除大多数HPV感染。该表提供了高风险类型(即癌症中发现的类型)的数据。
高危型HPV的清除率
初始阳性测试后数月8个月12个月18个月
测试阴性的男性百分比[105] 70%80%100%
如果有新的或持续的感染源,清除感染并不总能产生免疫力。赫尔南德斯2005年至2005年对25对夫妇进行的一项研究报告“在病毒清除后,许多情况表明[来自伴侣]明显再感染。”[77]
诊断
HPV有多种类型,有时称为“低风险”和“高风险”类型。低风险类型导致疣和高风险类型可导致病变或癌症。[106]
健康指南建议对具有特定适应症的患者进行HPV检测,包括某些异常的巴氏试验结果。
宫颈检查
根据国家癌症研究所的说法,“最常见的检测方法是检测几种高风险HPV类型的DNA,但它无法识别存在的类型。另一项测试特异于来自HPV 16和18型的DNA,这两种类型导致大多数HPV相关癌症。第三项测试可以检测来自几种高风险HPV类型的DNA,并可以指示是否存在HPV-16或HPV-18。第四项测试检测来自最常见的高风险HPV类型的RNA。这些测试可以在细胞异常明显之前检测HPV感染。
“从理论上讲,HPV DNA和RNA检测可用于鉴定从身体任何部位采集的细胞中的HPV感染。然而,这些测试仅获得FDA的批准,只有两种适应症:对30岁以上女性的宫颈癌检查结果和子宫颈癌筛查以及巴氏试验进行随访检测。“[107]
2011年4月,美国食品和药物管理局批准了由罗氏制造的cobas HPV测试。[108]该宫颈癌筛查试验“特异性识别HPV16和HPV18型,同时检测其余高风险类型(31,33,35,39,45,51,52,56,58,59,66和68)。 “[108]
在ATHENA试验中对cobas HPV试验进行了评估,该试验研究了超过47,000名21岁及以上的美国女性接受常规宫颈癌筛查。[109]来自ATHENA试验的结果显示,10名年龄在30岁及以上的女性中,有1名检测出HPV 16和/或18的阳性,实际上患有宫颈癌前期,即使他们在巴氏试验中显示正常结果[109]。
2003年3月,美国食品和药物管理局(FDA)批准了Qiagen / Digene制造的Hybrid Capture 2测试[110],这是一项“混合捕获”测试[111] [112],作为Pap测试的辅助手段。可以在常规巴氏涂片期间进行测试。它检测最常影响子宫颈的13种“高风险”HPV类型的DNA,但不确定特定的HPV类型。 Hybrid Capture 2是市场上研究最广泛的HPV检测方法,基于人群的筛查计划中HPV初级检测的大部分证据均基于Hybrid Capture 2检测。[113]
最近鉴定涉及宫颈癌的分子途径的结果提供了有关新型生物或致癌标志物的有用信息,这些标志物允许监测细胞学涂片,组织学或细胞学标本中的这些必需分子事件。这些生物标记物或癌基因标记物可能会改善初级筛查和分类设置中具有高进展风险的病变的检测。 E6和E7 mRNA检测PreTect HPV-Proofer(HPV OncoTect)或p16细胞周期蛋白水平是这些新分子标记的实例。根据已发表的结果,这些高度敏感和特异的标记物可以识别经历恶变的细胞。[114] [115]
2011年10月,美国食品和药物管理局批准了在任何HPV毒株开始产生癌症时产生的RNA的Aptima HPV Assay检测(见病毒学)。[116] [117] [118]
用Dacron拭子对外阴/阴道进行取样,显示出比子宫颈更多的HPV。在两个地区均为HPV阳性的女性中,90%在外阴阴道区域呈阳性,在宫颈中占46%。[81]
嘴巴测试
研究发现,患有口腔鳞状细胞癌的人的口腔细胞样本中的HPV升高。用牙刷(2,619个样本中的5个)[81]和细胞刷(未发现口腔传播)取样后,研究未发现口腔细胞中存在显着的HPV。[77]
测试男性
研究已经测试并发现了HPV,包括手指,口腔,唾液,肛门,尿道,尿液,精液,血液,阴囊和阴茎等高风险类型(即癌症中发现的类型)。然而,大多数研究测试都使用了Dacron拭子和普通大众无法获得的定制分析。[119]
巴西的一项研究使用了上面提到的现成的Qiagen / Digene测试(标签外)测试男性的阴茎,阴囊和肛门。[120] 50名男性中的每一个都是至少6个月的高危HPV阳性女性的伴侣。他们发现60%的男性患有高危HPV,主要是阴茎。 “在用生理盐水溶液喷洒肛门生殖器区域后,使用Digene试剂盒中包含的锥形刷的剧烈运动获得标本。”[120]
一种稍微不同的方法也使用了细胞刷(但是定制实验室分析),发现582名墨西哥军队招募了37%的高风险HPV阳性。[121] [需要更新]他们被告知在取样前12小时不要洗生殖器。 (其他研究没有提及洗涤,这是研究手中的一个特殊差距)。它们包括尿道以及阴囊和阴茎,但尿道的HPV率增加不到1%。像这样的研究使朱利亚诺建议对它们和阴囊之间的龟头,轴和折痕进行取样,因为尿道或肛门取样对诊断的影响很小。[79]邓恩推荐龟头,轴,皱褶和包皮。[119]
一项关于10名美国男性细胞刷的小型研究,其中刷子是湿的,而不是皮肤,发现10名男性中有2名HPV阳性(未报告类型)。[122] [需要更新]他们的实验室分析不同于要么在上面研究。这项小型研究发现,当用600粒砂纸擦拭皮肤时,10名男性中有4名为HPV阳性,然后用湿涤纶拭子擦拭。由于在实验室一起分析了金刚砂纸和刷子,因此不知道金刚砂纸是否收集病毒或将它们松开以便棉签收集。
研究发现,男性从自己的皮肤(用金刚砂纸和涤纶拭子)收集的效果与临床医生一样有效,有时甚至更多,因为患者更愿意大力刮擦。[123] [需要更新] [124] [125] ]
其他研究使用类似的细胞刷来取样指尖和指甲下,但没有弄湿区域或刷子。[80] [85] [126]
其他研究分析了尿液,精液和血液,发现了不同数量的HPV,[1​​19]但是没有公开的测试。
尽管HPV很常见,但没有广泛的测试。临床医生依赖于年轻人中的疫苗和高清除率(参见病毒学中的清除小节)来创造低风险的疾病和死亡率,并在癌症出现时对其进行治疗。其他人认为,即使没有任何症状,减少更多男性和女性的HPV感染也是重要的(群体免疫力),以防止更多的癌症,而不仅仅是治疗它们。[127] [128] [需要更新]在使用测试的地方,阴性测试结果显示传输的安全性,阳性测试结果显示需要屏蔽(避孕套,手套)以防止传播,直到感染清除。[129]
其他测试
虽然有可能在其他类型的感染中检测HPV DNA [130],但美国没有FDA批准的一般筛查测试[49]或加拿大政府批准的测试[131],因为测试是不确定,并认为在医学上没有必要。[132]
生殖器疣是低风险生殖器HPV的唯一可见迹象,可通过目视检查确定。然而,这些可见的生长是非致癌HPV类型的结果。百分之五的醋酸(醋)用于识别疣和鳞状上皮内瘤变(SIL)病变,并且通过使异常组织呈现白色而获得有限的成功,但大多数医生发现该技术仅在潮湿区域有用,例如作为女性生殖道。此时,男性的HPV检测仅用于研究。
已经进行了通过抗体存在测试HPV的研究。该方法正在寻找血液中的免疫反应,如果患者HPV阳性,其将包含HPV抗体。[133] [134] [135] [136]此类测试的可靠性尚未得到证实,因为截至2014年3月尚未获得FDA批准的产品;血液检测对于筛查目的来说是一种侵入性较小的检测。
预防
HPV疫苗可以预防最常见的感染类型。[3]为了有效,它们必须在感染发生之前使用,因此建议在9到13岁之间使用。宫颈癌筛查,例如使用Papanicolaou测试(pap)或在使用醋酸后观察子宫颈,可以检测可能发展成癌症的早期癌症或异常细胞。这允许早期治疗,从而产生更好的结果。[1]筛查减少了发达国家宫颈癌的死亡人数和死亡率。[10]疣可以通过冷冻去除。[4]
减少感染机会的方法包括性禁欲,避孕套和疫苗接种。[137]
疫苗
主要文章:HPV疫苗
有三种疫苗可用于预防某些HPV类型的感染:Gardasil,Cervarix和Gardasil 9.所有疫苗均可预防HPV 16和18型的初始感染,这些HPV引起大多数与HPV相关的癌症病例。 Gardasil还可以预防6型和11型HPV,这会导致90%的生殖器疣。 Gardasil是重组四价疫苗,而Cervarix是二价的,并且由L1衣壳蛋白的病毒样颗粒(VLP)制备。 Gardasil 9是非常的,它有可能预防约90%的宫颈癌,外阴癌,阴道癌和肛门癌。它可以保护6型,11型,16型,18型,31型,33型,45型,52型和58型HPV。后五种类型的宫颈癌可导致多达20%的宫颈癌,而这些癌症事先未被覆盖过。[138]
疫苗对已感染HPV 16和18型的妇女几乎没有益处。[139]因此,建议将疫苗主要用于那些在性行为期间尚未接触过HPV的女性。世界卫生组织关于HPV疫苗接种的立场文件明确概述了在公共部门计划中使用HPV疫苗的适当,具有成本效益的战略。[140]
有确凿的证据表明,HPV疫苗可预防年轻女性的宫颈癌前病变,特别是那些年龄在15至26岁之间的人。[141] HPV疫苗不会增加严重不良事件的风险。[142]需要更长时间的随访来监测HPV疫苗对子宫颈癌的影响。[142]
疾病预防控制中心建议疫苗分两次给药,间隔至少6个月,11至12岁的患者,以及年龄较大者的三剂。[143]在大多数国家,它们仅供女性使用,但在许多国家被批准用于男性,并为澳大利亚的十几岁男孩提供资助。该疫苗对现有的HPV感染或宫颈病变没有任何治疗效果。[144] 2010年,美国49%的少女接种了HPV疫苗。
根据研究表明,疫苗对年轻女孩[145]比年龄较大的女孩更有效,英国,瑞士,墨西哥,荷兰和魁北克开始为2014年15岁以下女孩提供两剂疫苗。
对于接种HPV疫苗的女性,宫颈癌筛查建议没有改变。仍然建议妇女即使在接种疫苗后仍继续接受子宫颈检查,例如子宫颈抹片检查,因为它不能预防所有类型的宫颈癌。[144] [146]
男性和女性都是HPV的携带者。[147] Gardasil疫苗还可以保护男性免受肛门癌,疣和生殖器疣的侵害。[148]
自从它们首次开发以来,已经观察到两种疫苗的功效持续时间,并且预计它们是持久的。[149]
2014年12月,FDA批准了一种基于Gardasil的9价疫苗Gardasil 9,以防止第一代Gardasil覆盖的4种HPV感染以及5种其他负责20%宫颈癌的菌株感染( HPV-31,HPV-33,HPV-45,HPV-52和HPV-58)。[150]
避孕套
美国疾病控制和预防中心表示,男性“使用安全套可降低生殖器人​​乳头瘤病毒(HPV)感染的风险”,但与其他性传播疾病相比,其提供的保护程度较低,因为HPV也可通过暴露于地区传播(例如,受感染的皮肤或粘膜表面)未被避孕套覆盖或保护。“[151]
女用避孕套比男用避孕套提供更大的保护,因为女用避孕套可以减少皮肤接触。[152]
研究表明,定期使用安全套可以有效地限制HPV持续存在并扩散到已感染个体的其他生殖器部位。[需要更新]
消毒
该病毒相对耐寒,对许多常见的消毒剂免疫。暴露于90%乙醇至少1分钟,2%戊二醛,30%Savlon和/或1%次氯酸钠可以对病原体进行消毒。[153]
该病毒耐干燥和耐热,但在100°C(212°F)和紫外线辐射下会被杀死。[153]
治疗
另见:生殖器疣
目前尚无针对HPV感染的具体治疗方法。[154] [155] [156]然而,病毒感染通常会自行清除到无法察觉的水平。[157]根据疾病控制和预防中心的说法,身体的免疫系统可以在两年内自然清除HPV 90%的病例(详见病毒学中的清除小节)。[154]但是,专家们不同意病毒是否被完全消除或降至不可检测的水平,并且很难知道它何时具有传染性。[158]
许多诊所通常建议并实施后续护理。[159]随访有时不成功,因为一部分受治疗者不会返回进行评估。除了通常的电话和邮件方法外,短信和电子邮件还可以改善返回护理的人数。[160]
流行病学
据估计,在世界范围内,HPV在任何特定时间都会感染约12%的女性。[161] HPV感染是世界上最常见的性传播疾病。[162]
美国
按年龄分列的女性HPV患病率,包括20种低风险类型和23种高风险类型[163]
HPV估计是美国最常见的性传播感染。[163]大多数性活跃的男性和女性可能会在生命中的某些时候感染生殖器HPV。[40]美国社会健康协会估计,大约75-80%的性活跃美国人将在其一生中的某个时间点感染HPV。[164] [165]到50岁时,超过80%的美国女性将至少感染一种生殖器HPV。[163] [166]据估计,在2000年,15-44岁的美国人中有大约620万新的HPV感染;其中,估计有74%发生在15至24岁之间的人中。[167]在研究的性传播疾病中,生殖器HPV是最常见的。[167]在美国,估计有10%的人口有HPV感染,4%有感染引起细胞学异常,另有1%有感染引起生殖器疣。[168]
HPV患病率估计值从14%到90%不等。[169]造成这种差异的一个原因是,一些研究报告了目前可检测到感染的妇女,而其他研究则报告了曾经有过可检测感染的妇女。[170] [171]差异的另一个原因是测试的菌株差异。
一项研究发现,在2003 - 2004年期间,在任何特定时间,26.8%的14至59岁女性至少感染了一种HPV。这比以前的估计高; 15.2%感染了一种或多种可导致癌症的高风险类型。[163] [172]
高风险和低风险类型的患病率随着时间的推移大致相似。[163]
人乳头瘤病毒不包括在2011年通常可向CDC报告的疾病中。[173] [174]
历史
1972年,StefaniaJabłońska在波兰提出了人乳头瘤病毒与皮肤癌在表皮发育不良中的关联。 1978年,巴斯德研究所的Jabłońska和Gerard Orth在皮肤癌中发现了HPV-5 [175] [页码需要] 1976年,Harald zur Hausen发表了人类乳头状瘤病毒在宫颈癌病因中发挥重要作用的假设。 1983年和1984年,祖尔·豪森和他的合作者在宫颈癌中发现了HPV16和HPV18。[176]
HeLa细胞系在其基因组中含有来自HPV18型的额外DNA。[177]
研究
Ludwig-McGill HPV队列,对人乳头瘤病毒感染和宫颈癌风险自然史的大型纵向研究
一项研究发现了支持大蒜提取物的初步证据。[178]
参考:
1. "Human papillomavirus (HPV) and cervical cancer". WHO. June 2016. Archived from the original on 5 August 2016. Retrieved 10 August 2016.
2. Ljubojevic, Suzana; Skerlev, Mihael (2014). "HPV-associated diseases". Clinics in Dermatology. 32 (2): 227–234. doi:10.1016/j.clindermatol.2013.08.007. ISSN 0738-081X. PMID 24559558.
3. "What is HPV?". CDC. 28 December 2015. Archived from the original on 7 August 2016. Retrieved 10 August 2016.
4. Milner, Danny A. (2015). Diagnostic Pathology: Infectious Diseases. Elsevier Health Sciences. p. 40. ISBN 9780323400374. Archived from the original on 11 September 2017.
5. "Fact Sheet for Public Health Personnel | Condom Effectiveness | CDC". www.cdc.gov. 25 March 2013. Archived from the original on 27 May 2017. Retrieved 1 May 2017.
6. "The Link Between HPV and Cancer". CDC. September 30, 2015. Archived from the original on 9 November 2015. Retrieved 11 August 2016.
7. Bzhalava, D; Guan, P; Franceschi, S; Dillner, J; Clifford, G (2013), "A systematic review of the prevalence of mucosal and cutaneous human papillomavirus types", Virology, 445 (1–2): 224–31, doi:10.1016/j.virol.2013.07.015, PMID 23928291
8. "Human Papillomavirus (HPV) Questions and Answers". CDC. 28 December 2015. Archived from the original on 11 August 2016. Retrieved 11 August 2016.
9. "Pink Book (Human Papillomavirus)" (PDF). CDC.gov. Archived (PDF) from the original on 21 March 2017. Retrieved 18 April 2017.
10. Sawaya, GF; Kulasingam, S; Denberg, TD; Qaseem, A; Clinical Guidelines Committee of American College of, Physicians (16 June 2015). "Cervical Cancer Screening in Average-Risk Women: Best Practice Advice From the Clinical Guidelines Committee of the American College of Physicians". Annals of Internal Medicine. 162 (12): 851–9. doi:10.7326/M14-2426. PMID 25928075. Archived from the original on 5 May 2015.
11. World Cancer Report 2014. World Health Organization. 2014. pp. Chapter 5.12. ISBN 9283204298.
12. Tyring, Stephen; Moore, Angela Yen; Lupi, Omar (2016). Mucocutaneous Manifestations of Viral Diseases: An Illustrated Guide to Diagnosis and Management (2 ed.). CRC Press. p. 207. ISBN 9781420073133.
13. EHPV, archived from the original on 17 December 2014
14. Chaturvedi, Anil; Maura L. Gillison (4 March 2010). "Human Papillomavirus and Head and Neck Cancer". In Andrew F. Olshan. Epidemiology, Pathogenesis, and Prevention of Head and Neck Cancer (1st ed.). New York: Springer. ISBN 978-1-4419-1471-2.
15. Muñoz, N; Bosch, F. X.; De Sanjosé, S; Herrero, R; Castellsagué, X; Shah, K. V.; Snijders, P. J.; Meijer, C. J.; International Agency for Research on Cancer Multicenter Cervical Cancer Study Group (2003), "Epidemiologic classification of human papillomavirus types associated with cervical cancer", The New England Journal of Medicine, 348 (6): 518–27, doi:10.1056/NEJMoa021641, PMID 12571259, archived from the original on 30 April 2012
16. Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Mitchell, Richard (2007). "Chapter 19 The Female Genital System and Breast". Robbins Basic Pathology (8 ed.). Philadelphia: Saunders. ISBN 1-4160-2973-7.
17. Palefsky, Joel M.; Holly, Elizabeth A.; Ralston, Mary L.; Jay, Naomi (February 1988). "Prevalence and Risk Factors for Human Papillomavirus Infection of the Anal Canal in Human Immunodeficiency Virus (HIV)–Positive and HIV-Negative Homosexual Men" (PDF). Departments of Laboratory Medicine, Stomatology, and Epidemiology Biostatistics, University of California, San Francisco. The Journal of Infectious Diseases Oxford University Press. Archived from the original on 15 January 2013. Retrieved 2 March 2014.
18. Muñoz N, Castellsagué X, de González AB, Gissmann L; Castellsagué; De González (2006). "Chapter 1: HPV in the etiology of human cancer". Vaccine. 24 (3): S1–S10. doi:10.1016/j.vaccine.2006.05.115. PMID 16949995.
19. Antonsson A, Forslund O, Ekberg H, Sterner G, Hansson BG (2000). "The ubiquity and impressive genomic diversity of human skin papillomaviruses suggest a commensalic nature of these viruses". J. Virol. 74 (24): 11636–41. doi:10.1128/JVI.74.24.11636-11641.2000. PMC 112445 Freely accessible. PMID 11090162.
20. Mayo Clinic.com, Common warts, http://www.mayoclinic.com/print/ ... ON=all&METHOD=print Archived 17 October 2011 at the Wayback Machine.
21. De Koning MN, Quint KD, Bruggink SC, Gussekloo J, Bouwes Bavinck JN, Feltkamp MC, Quint WG, Eekhof JA (2014). "High prevalence of cutaneous warts in elementary school children and ubiquitous presence of wart-associated HPV on clinically normal skin". The British Journal of Dermatology. 172: 196–201. doi:10.1111/bjd.13216. PMID 24976535.
22. Lountzis NI, Rahman O (2008). "Images in clinical medicine. Digital verrucae". N. Engl. J. Med. 359 (2): 177. doi:10.1056/NEJMicm071912. PMID 18614785.
23. MedlinePlus, Warts, https://www.nlm.nih.gov/medlineplus/warts.html#cat42 Archived 5 June 2016 at the Wayback Machine. (general reference with links). Also, see
24. Greer CE, Wheeler CM, Ladner MB, Beutner K, Coyne MY, Liang H, Langenberg A, Yen TS, Ralston R (1995). "Human papillomavirus (HPV) type distribution and serological response to HPV type 6 virus-like particles in patients with genital warts". J. Clin. Microbiol. 33 (8): 2058–63. PMC 228335 Freely accessible. PMID 7559948.
25. "Human Papillomavirus". Medscape. Archived from the original on 29 November 2016.
26. "Photos of larynx Papillomas — Voice Medicine, New York". Voicemedicine.com. Archived from the original on 12 June 2010. Retrieved 29 August 2010.
27. Sinal SH, Woods CR (2005). "Human papillomavirus infections of the genital and respiratory tracts in young children". Seminars in Pediatric Infectious Diseases. 16 (4): 306–16. doi:10.1053/j.spid.2005.06.010. PMID 16210110.
28. Wu R, Sun S, Steinberg BM (2003). "Requirement of STAT3 activation for differentiation of mucosal stratified squamous epithelium". Mol. Med. 9 (3–4): 77–84. doi:10.2119/2003-00001.Wu. PMC 1430729 Freely accessible. PMID 12865943.
29. Moore CE, Wiatrak BJ, McClatchey KD, Koopmann CF, Thomas GR, Bradford CR, Carey TE (1999). "High-risk human papillomavirus types and squamous cell carcinoma in patients with respiratory papillomas". Otolaryngol. Head Neck Surg. 120 (5): 698–705. doi:10.1053/hn.1999.v120.a91773. PMID 10229596.
30. Parkin DM (2006). "The global health burden of infection-associated cancers in the year 2002". Int. J. Cancer. 118 (12): 3030–44. doi:10.1002/ijc.21731. PMID 16404738.
31. Pahud, BA; Ault, KA (December 2015). "The Expanded Impact of Human Papillomavirus Vaccine". Infectious Disease Clinics of North America (Review). 29 (4): 715–24. doi:10.1016/j.idc.2015.07.007. PMID 26610422.
32. Nowińska, K; Ciesielska, U; Podhorska-Okołów, M; Dzięgiel, P (2017). "The role of human papillomavirus in oncogenic transformation and its contribution to the etiology of precancerous lesions and cancer of the larynx: A review". Advances in clinical and experimental medicine : official organ Wroclaw Medical University. 26 (3): 539–547. doi:10.17219/acem/67461. PMID 28791831.
33. "Archived copy". Archived from the original on 24 August 2012. Retrieved 24 August 2012.(subscription required)[clarification needed]
34. Schiffman M, Castle PE (2005). "The promise of global cervical-cancer prevention". N. Engl. J. Med. 353 (20): 2101–4. doi:10.1056/NEJMp058171. PMID 16291978.
35. Alam S, Conway MJ, Chen HS, Meyers C (2007). "Cigarette Smoke Carcinogen Benzo[a]pyrene Enhances Human Papillomavirus Synthesis". J Virol. 82 (2): 1053–8. doi:10.1128/JVI.01813-07. PMC 2224590 Freely accessible. PMID 17989183.
36. Lu B, Hagensee ME, Lee JH, Wu Y, Stockwell HG, Nielson CM, Abrahamsen M, Papenfuss M, Harris RB, Giuliano AR (February 2010). "Epidemiologic factors associated with seropositivity to human papillomavirus type 16 and 18 virus-like particles and risk of subsequent infection in men". Cancer Epidemiol. Biomarkers Prev. 19 (2): 511–6. doi:10.1158/1055-9965.EPI-09-0790. PMID 20086109.
37. Liu, Ying (2015). "Comprehensive mapping of the human papillomavirus (HPV) DNA integration sites in cervical carcinomas by HPV capture technology". Oncotarget. 7: 5852–5864. doi:10.18632/oncotarget.6809. PMC 4868726 Freely accessible. PMID 26735580.
38. Parfenov, Michael (2014). "Characterization of HPV and host genome interactions in primary head and neck cancers". Proceedings of the National Academy of Sciences. 111: 15544–15549. doi:10.1073/pnas.1416074111. PMC 4217452 Freely accessible. PMID 25313082.
39. Karagas MR, Waterboer T, Li Z, Nelson HH, Michael KM, Bavinck JN, Perry AE, Spencer SK, Daling J, Green AC, Pawlita M (2010). "Genus β human papillomaviruses and incidence of basal cell and squamous cell carcinomas of skin: population based case-control study". BMJ. 341: 2986. doi:10.1136/bmj.c2986. PMC 2900549 Freely accessible. PMID 20616098. Archived from the original on 15 July 2010.
40. Baseman JG, Koutsky LA (2005). "The epidemiology of human papillomavirus infections". J. Clin. Virol. 32 (Suppl 1): S16–24. doi:10.1016/j.jcv.2004.12.008. PMID 15753008. Overall, these DNA-based studies, combined with measurements of type-specific antibodies against HPV capsid antigens, have shown that most (>50%) sexually active women have been infected by one or more genital HPV types at some point in time [S17].
41. Cohen J (2005). "Public health. High hopes and dilemmas for a cervical cancer vaccine". Science. 308 (5722): 618–21. doi:10.1126/science.308.5722.618. PMID 15860602.
42. Ault KA (2006). "Epidemiology and Natural History of Human Papillomavirus Infections in the Female Genital tract". Infectious Diseases in Obstetrics and Gynecology. 2006: 1–5. doi:10.1155/IDOG/2006/40470. PMC 1581465 Freely accessible. PMID 16967912.
43. Kreimer, Aimee R.; Clifford, Gary M.; Boyle, Peter; Franceschi, Silvia (1 February 2005). "Human papillomavirus types in head and neck squamous cell carcinomas worldwide: a systematic review". Cancer Epidemiology, Biomarkers & Prevention. 14 (2): 467–475. doi:10.1158/1055-9965.EPI-04-0551. ISSN 1055-9965. PMID 15734974.
44. Noel J, Lespagnard L, Fayt I, Verhest A, Dargent J (2001). "Evidence of human papilloma virus infection but lack of Epstein-Barr virus in lymphoepithelioma-like carcinoma of uterine cervix: report of two cases and review of the literature". Hum. Pathol. 32 (1): 135–8. doi:10.1053/hupa.2001.20901. PMID 11172309.
45. "Vulvar Intraepithelial Neoplasia: Varied signs, varied symptoms: what you need to know". www.advanceweb.com. Archived from the original on 16 July 2012. Retrieved 5 August 2009.
46. Bolt J, Vo QN, Kim WJ, McWhorter AJ, Thomson J, Hagensee ME, Friedlander P, Brown KD, Gilbert J (2005). "The ATM/p53 pathway is commonly targeted for inactivation in squamous cell carcinoma of the head and neck (SCCHN) by multiple molecular mechanisms". Oral Oncol. 41 (10): 1013–20. doi:10.1016/j.oraloncology.2005.06.003. PMID 16139561.
47. Greenblatt, R. J. (2005). "Human papillomaviruses: Diseases, diagnosis, and a possible vaccine". Clinical Microbiology Newsletter. 27 (18): 139–145. doi:10.1016/j.clinmicnews.2005.09.001.
48. Freitas LB, Chen Z, Muqui EF, Boldrini NA, Miranda AE, Spano LC, Burk RD (2014-07-01). "Human Papillomavirus 16 Non-European Variants Are Preferentially Associated with High-Grade Cervical Lesions". PLOS ONE. 9: e100746. doi:10.1371/journal.pone.0100746. PMC 4077691 Freely accessible. PMID 24983739.
49. "HPV and Men — CDC Fact Sheet". Centers for Disease Control and Prevention (CDC). 3 April 2008. Archived from the original on 17 October 2009. Retrieved 13 November 2009.
50. Frisch M, Smith E, Grulich A, Johansen C (2003). "Cancer in a population-based cohort of men and women in registered homosexual partnerships". Am. J. Epidemiol. 157 (11): 966–72. doi:10.1093/aje/kwg067. PMID 12777359. Archived from the original on 19 May 2009. However, the risk for invasive anal squamous carcinoma, which is believed to be caused by certain types of sexually transmitted human papillomaviruses, a notable one being type 16, was significantly 31-fold elevated at a crude incidence of 25.6 per 100,000 person-years
51. Thomas W. Gaither; et al. (2015). "The Influence of Sexual Orientation and Sexual Role on Male Grooming-Related Injuries and Infections". J Sex Med. 12 (3): 631–640. doi:10.1111/jsm.12780. PMC 4599875 Freely accessible.
52. Chin-Hong PV, Vittinghoff E, Cranston RD, Browne L, Buchbinder S, Colfax G, Da Costa M, Darragh T, Benet DJ, Judson F, Koblin B, Mayer KH, Palefsky JM (2005). "Age-related prevalence of anal cancer precursors in homosexual men: the EXPLORE study". J. Natl. Cancer Inst. 97 (12): 896–905. doi:10.1093/jnci/dji163. PMID 15956651.
53. "AIDSmeds Web Exclusives : Pap Smears for Anal Cancer? — by David Evans". AIDSmeds.com. Archived from the original on 7 July 2011. Retrieved 29 August 2010.
54. Goldie SJ, Kuntz KM, Weinstein MC, Freedberg KA, Palefsky JM (June 2000). "Cost-effectiveness of screening for anal squamous intraepithelial lesions and anal cancer in human immunodeficiency virus-negative homosexual and bisexual men". Am. J. Med. 108 (8): 634–41. doi:10.1016/S0002-9343(00)00349-1. PMID 10856411.
55. Gillison ML, Koch WM, Capone RB, Spafford M, Westra WH, Wu L, Zahurak ML, Daniel RW, Viglione M, Symer DE, Shah KV, Sidransky D (2000). "Evidence for a causal association between human papillomavirus and a subset of head and neck cancers". J. Natl. Cancer Inst. 92 (9): 709–20. doi:10.1093/jnci/92.9.709. PMID 10793107.
56. Gillison ML (2006). "Human papillomavirus and prognosis of oropharyngeal squamous cell carcinoma: implications for clinical research in head and neck cancers". J. Clin. Oncol. 24 (36): 5623–5. doi:10.1200/JCO.2006.07.1829. PMID 17179099.
57. D'Souza G, Kreimer AR, Viscidi R, Pawlita M, Fakhry C, Koch WM, Westra WH, Gillison ML (2007). "Case-control study of human papillomavirus and oropharyngeal cancer". N. Engl. J. Med. 356 (19): 1944–56. doi:10.1056/NEJMoa065497. PMID 17494927. Archived from the original on 12 May 2007.
58. Ridge JA, Glisson BS, Lango MN, et al. "Head and Neck Tumors" Archived 20 July 2009 at the Wayback Machine. in Pazdur R, Wagman LD, Camphausen KA, Hoskins WJ (Eds) Cancer Management: A Multidisciplinary Approach Archived 4 October 2013 at the Wayback Machine.. 11 ed. 2008.
59. "Oral Cancer on the rise among non-smokers under 50" (PDF). California Dental Hygienists’ Association. Archived from the original (PDF) on 24 January 2011. Retrieved 10 January 2011.
60. Chaturvedi, Anil K.; Engels, Eric A.; Pfeiffer, Ruth M.; Hernandez, Brenda Y.; Xiao, Weihong; Kim, Esther; Jiang, Bo; Goodman, Marc T.; Sibug-Saber, Maria (10 November 2011). "Human papillomavirus and rising oropharyngeal cancer incidence in the United States". Journal of Clinical Oncology. 29 (32): 4294–4301. doi:10.1200/JCO.2011.36.4596. ISSN 1527-7755. PMC 3221528 Freely accessible. PMID 21969503.
61. Chaturvedi AK, Engels EA, Pfeiffer RM, Hernandez BY, Xiao W, Kim E, Jiang B, Goodman MT, Sibug-Saber M, Cozen W, Liu L, Lynch CF, Wentzensen N, Jordan RC, Altekruse S, Anderson WF, Rosenberg PS, Gillison ML (October 2011). "Human Papillomavirus and Rising Oropharyngeal Cancer Incidence in the United States". Journal of Clinical Oncology. 29 (32): 4294–301. doi:10.1200/JCO.2011.36.4596. PMC 3221528 Freely accessible. PMID 21969503.
62. Ernster JA, Sciotto CG, O'Brien MM, Finch JL, Robinson LJ, Willson T, Mathews M (December 2007). "Rising incidence of oropharyngeal cancer and the role of oncogenic human papilloma virus". The Laryngoscope. 117 (12): 2115–28. doi:10.1097/MLG.0b013e31813e5fbb. PMID 17891052.
63. Kidon MI, Shechter E, Toubi E (January 2011). "[Vaccination against human papilloma virus and cervical cancer]". Harefuah (in Hebrew). 150 (1): 33–6, 68. PMID 21449154.
64 Lechner M, Frampton GM, Fenton T, Feber A, Palmer G, Jay A, Pillay N, Forster M, Cronin MT, Lipson D, Miller VA, Brennan TA, Henderson S, Vaz F, O'Flynn P, Kalavrezos N, Yelensky R, Beck S, Stephens PJ, Boshoff C, Boshoff G (2013). "Targeted next-generation sequencing of head and neck squamous cell carcinoma identifies novel genetic alterations in HPV+ and HPV- tumors". Genome Medicine. 5 (5): 49. doi:10.1186/gm453. PMC 4064312 Freely accessible. PMID 23718828.
65. "Lung Cancer Risk Rises in the Presence of HPV Antibodies". Lung Cancer Risk Rises in the Presence of HPV Antibodies. Archived from the original on 27 April 2012.
66. "Lung Cancer Patients More Likely to Have High-Risk Human Papillomavirus". NPIN. Archived from the original on 27 July 2012.
67. Syrjänen K, Syrjänen S, Kellokoski J, Kärjä J, Mäntyjärvi R (1989). "Human papillomavirus (HPV) type 6 and 16 DNA sequences in bronchial squamous cell carcinomas demonstrated by in situ DNA hybridization". Lung. 167 (1): 33–42. doi:10.1007/BF02714928. PMID 2537916.
68. Carpagnano GE, Koutelou A, Natalicchio MI, Martinelli D, Ruggieri C, Di Taranto A, Antonetti R, Carpagnano F, Foschino-Barbaro MP (11 October 2011). "HPV in exhaled breath condensate of lung cancer patients". British Journal of Cancer. 105 (8): 1183–90. doi:10.1038/bjc.2011.354. PMC 3208494 Freely accessible. PMID 21952627.
69. Klein F, Amin Kotb WF, Petersen I (July 2009). "Incidence of human papillomavirus in lung cancer". Lung Cancer. 65 (1): 13–8. doi:10.1016/j.lungcan.2008.10.003. PMID 19019488.
70. Moore, Matthew (12 November 2007). "Tree man 'who grew roots' may be cured". The Daily Telegraph. London. Archived from the original on 13 November 2007.
71. "HPV and Cancer". National Cancer Institute. Archived from the original on 18 April 2017. Retrieved 18 April 2017.
72. Heymann, MD, David (2015). Control of Communicable Diseases Manual (20th ed.). Washington D.C.: Apha Press. pp. 299–300. ISBN 978-0-87553-018-5.
73. Burchell AN, Winer RL, de Sanjosé S, Franco EL (Aug 2006). "Chapter 6: Epidemiology and transmission dynamics of genital HPV infection". Vaccine. 24 Suppl 3: S3/52–61. doi:10.1016/j.vaccine.2006.05.031. ISSN 0264-410X. PMID 16950018.
74. Schmitt M, Depuydt C, Benoy I, Bogers J, Antoine J, Arbyn M, Pawlita M (2012). "Prevalence and viral load of 51 genital human papillomavirus types and 3 subtypes". Int J Cancer. 132: 2395–2403. doi:10.1002/ijc.27891.
75. Muñoz N, Bosch FX, de Sanjosé S, Herrero R, Castellsagué X, Shah KV, Snijders PJ, Meijer CJ (2003). "Epidemiologic classification of human papillomavirus types associated with cervical cancer". N. Engl. J. Med. 348 (6): 518–27. doi:10.1056/NEJMoa021641. PMID 12571259.
76. Egendorf, Laura. Sexually Transmitted Diseases (At Issue Series). New York: Greenhaven Press, 2007.
77. Hernandez BY, Wilkens LR, Zhu X, Thompson P, McDuffie K, Shvetsov YB, Kamemoto LE, Killeen J, Ning L, Goodman MT (2008). "Transmission of human papillomavirus in heterosexual couples". Emerging Infectious Diseases. 14 (6): 888–894. doi:10.3201/eid1406.070616. PMC 2600292 Freely accessible. PMID 18507898.
78. Hernandez BY, Wilkens LR, Zhu X, et al. (June 2008). "Transmission of human papillomavirus in heterosexual couples" (PDF). Emerging Infect. Dis. 14: 888–94. doi:10.3201/eid1406.070616. PMC 2600292 Freely accessible. PMID 18507898. Archived (PDF) from the original on 23 July 2017.
79. Giuliano AR, Nielson CM, Flores R, Dunne EF, Abrahamsen M, Papenfuss MR, Markowitz LE, Smith D, Harris RB (2007). "The Optimal Anatomic Sites for Sampling Heterosexual Men for Human Papillomavirus (HPV) Detection: The HPV Detection in Men Study". The Journal of Infectious Diseases. 196 (8): 1146–1152. doi:10.1086/521629. PMC 3904649 Freely accessible. PMID 17955432.
80. Winer RL, Hughes JP, Feng Q, Xi LF, Cherne S, O'Reilly S, Kiviat NB, Koutsky LA (2010). "Detection of genital hpv types in fingertip samples from newly sexually active female university students". Cancer Epidemiology Biomarkers & Prevention. 19 (7): 1682–1685. doi:10.1158/1055-9965.EPI-10-0226. PMC 2901391 Freely accessible. PMID 20570905.
81. Winer RL, Lee SK, Hughes JP, Adam DE, Kiviat NB, Koutsky LA (2003). "Genital human papillomavirus infection: Incidence and risk factors in a cohort of female university students". American Journal of Epidemiology. 157 (3): 218–226. doi:10.1093/aje/kwf180. PMID 12543621.
82. Tay SK (Jul 1995). "Genital oncogenic human papillomavirus infection: a short review on the mode of transmission" (Free full text). Annals of the Academy of Medicine, Singapore. 24 (4): 598–601. ISSN 0304-4602. PMID 8849195. Archived from the original on 27 July 2012.
83. Pao CC, Tsai PL, Chang YL, Hsieh TT, Jin JY (Mar 1993). "Possible non-sexual transmission of genital human papillomavirus infections in young women". European Journal of Clinical Microbiology & Infectious Diseases. 12 (3): 221–222. doi:10.1007/BF01967118. ISSN 0934-9723. PMID 8389707.
84. Tay SK, Ho TH, Lim-Tan SK (Aug 1990). "Is genital human papillomavirus infection always sexually transmitted?" (Free full text). The Australian & New Zealand Journal of Obstetrics & Gynaecology. 30 (3): 240–242. doi:10.1111/j.1479-828X.1990.tb03223.x. ISSN 0004-8666. PMID 2256864. Archived from the original on 6 April 2016.
85. Sonnex C, Strauss S, Gray JJ (October 1999). "Detection of human papillomavirus DNA on the fingers of patients with genital warts". Sexually Transmitted Infections. 75 (5): 317–319. doi:10.1136/sti.75.5.317. ISSN 1368-4973. PMC 1758241 Freely accessible. PMID 10616355.
86. Hans Krueger; Gavin Stuart; Richard Gallagher; Dan Williams, Jon Kerner (12 April 2010). HPV and Other Infectious Agents in Cancer:Opportunities for Prevention and Public Health: Opportunities for Prevention and Public Health. Oxford University Press. p. 34. ISBN 978-0-19-973291-3. Archived from the original on 9 June 2013. Retrieved 24 December 2012.
87. Bodaghi S, Wood LV, Roby G, Ryder C, Steinberg SM, Zheng ZM (November 2005). "Could human papillomaviruses be spread through blood?". J. Clin. Microbiol. 43 (11): 5428–34. doi:10.1128/JCM.43.11.5428-5434.2005. PMC 1287818 Freely accessible. PMID 16272465.
88. Chen AC, Keleher A, Kedda MA, Spurdle AB, McMillan NA, Antonsson A (October 2009). "Human papillomavirus DNA detected in peripheral blood samples from healthy Australian male blood donors". J. Med. Virol. 81 (10): 1792–6. doi:10.1002/jmv.21592. PMID 19697401.
89. "Eligibility Criteria by Topic - American Red Cross". Archived from the original on 1 January 2017.
90. Watson RA (2005). "Human Papillomavirus: Confronting the Epidemic—A Urologist's Perspective". Rev Urol. 7: 135–44. PMC 1477576 Freely accessible. PMID 16985824.
91. Schiller JT, Day PM, Kines RC (2010). "Current understanding of the mechanism of HPV infection". Gynecologic Oncology. 118 (1 Suppl): S12. doi:10.1016/j.ygyno.2010.04.004. PMC 3493113 Freely accessible. PMID 20494219.
92. Scheurer ME, Tortolero-Luna G, Adler-Storthz K (2005). "Human papillomavirus infection: biology, epidemiology, and prevention". International Journal of Gynecological Cancer. 15 (5): 727–746. doi:10.1111/j.1525-1438.2005.00246.x. PMID 16174218.
93. Woodham, Andrew W.; Da Silva, Diane M.; Skeate, Joseph G.; Raff, Adam B.; Ambroso, Mark R.; Brand, Heike E.; Isas, J. Mario; Langen, Ralf; Kast, W. Martin (2012). "The S100A10 subunit of the annexin A2 heterotetramer facilitates L2-mediated human papillomavirus infection". PLoS One. 7 (8): e43519. doi:10.1371/journal.pone.0043519. ISSN 1932-6203. PMC 3425544 Freely accessible. PMID 22927980.
94. Raff, Adam B.; Woodham, Andrew W.; Raff, Laura M.; Skeate, Joseph G.; Yan, Lisa; Da Silva, Diane M.; Schelhaas, Mario; Kast, W. Martin (June 2013). "The evolving field of human papillomavirus receptor research: a review of binding and entry". Journal of Virology. 87 (11): 6062–6072. doi:10.1128/JVI.00330-13. ISSN 1098-5514. PMC 3648114 Freely accessible. PMID 23536685.
95. Chen Z, Schiffman M, Herrero R, Desalle R, Anastos K, Segondy M, Sahasrabuddhe VV, Gravitt PE, Hsing AW, Burk RD (2011). "Evolution and Taxonomic Classification of Human Papillomavirus 16 (HPV16)-Related Variant Genomes". PLOS ONE. 6 (5): 1–16. doi:10.1371/journal.pone.0020183. PMC 3103539 Freely accessible. PMID 21673791.
96. Zuna RE, Tuller E, Wentzensen N, Mathews C, Allen RA, Shanesmith R, Dunn ST, Gold MA, Wang SS, Walker J, Schiffman M (2011). "HPV16 Variant Lineage, Clinical Stage, And Survival in Women With Invasive Cervical Cancer". Infectious Agents & Cancer. 6: 19–27. doi:10.1186/1750-9378-6-19. PMC 3226431 Freely accessible. PMID 22035468.
97. Ganguly N, Parihar SP (2009). "Human papillomavirus E6 and E7 oncoproteins as risk factors for tumorigenesis". Journal of Biosciences. 34 (1): 113–123. doi:10.1007/s12038-009-0013-7. PMID 19430123.
98. Zheng ZM, Baker CC (2006). "Papillomavirus genome structure, expression, and post-transcriptional regulation". Frontiers in Bioscience. 11: 2286–2302. doi:10.2741/1971. PMC 1472295 Freely accessible. PMID 16720315.
99. Tang S, Tao M, McCoy JP, Zheng ZM (2006). "The E7 Oncoprotein is Translated from Spliced E6*I Transcripts in High-Risk Human Papillomavirus Type 16- or Type 18-Positive Cervical Cancer Cell Lines via Translation Reinitiation". Journal of Virology. 80 (9): 4249–4263. doi:10.1128/JVI.80.9.4249-4263.2006. PMC 1472016 Freely accessible. PMID 16611884.
100. Münger K, Howley PM (2002). "Human papillomavirus immortalization and transformation functions". Virus Research. 89 (2): 213–228. doi:10.1016/S0168-1702(02)00190-9. PMID 12445661.
101. Conway MJ, Alam S, Ryndock EJ, Cruz L, Christensen ND, Roden RB, Meyers C (October 2009). "Tissue-spanning redox gradient-dependent assembly of native human papillomavirus type 16 virions". Journal of Virology. 83 (20): 10515–26. doi:10.1128/JVI.00731-09. PMC 2753102 Freely accessible. PMID 19656879.
102. Bryan JT, Brown DR (March 2001). "Transmission of human papillomavirus type 11 infection by desquamated cornified cells". Virology. 281 (1): 35–42. doi:10.1006/viro.2000.0777. PMID 11222093.
103. Rampias T, Boutati E, Pectasides E, Sasaki C, Kountourakis P, Weinberger P, Psyrri A (2010). "Activation of Wnt signaling pathway by human papillomavirus E6 and E7 oncogenes in HPV16-positive oropharyngeal squamous carcinoma cells". Molecular Cancer Research. 8 (3): 433–443. doi:10.1158/1541-7786.MCR-09-0345. PMID 20215420.
104. Watson RA (2005). "Human Papillomavirus: Confronting the Epidemic—A Urologist's Perspective". Reviews in Urology. 7 (3): 135–44. PMC 1477576 Freely accessible. PMID 16985824.
105. Giuliano AR, Lu B, Nielson CM, Flores R, Papenfuss MR, Lee JH, Abrahamsen M, Harris RB (2008). "Age‐Specific Prevalence, Incidence, and Duration of Human Papillomavirus Infections in a Cohort of 290 US Men". The Journal of Infectious Diseases. 198 (6): 827–835. doi:10.1086/591095. PMID 18657037.
106. Schiffman M, Castle PE; Castle (August 2003). "Human papillomavirus: epidemiology and public health" [1 January 2017]. Arch. Pathol. Lab. Med. 127 (8): 930–4. doi:10.1043/1543-2165(2003)127<930:HPEAPH>2.0.CO;2. ISSN 1543-2165. PMID 12873163. Archived from the original on 2013-04-14.
107. "National Cancer Institute Fact Sheet: HPV and Cancer". Cancer.gov. Archived from the original on 31 October 2013. Retrieved 23 October 2013.
108. "FDA Approval of cobas HPV Test – P1000020". U.S Food and Drug Administration. Archived from the original on 15 February 2013. Retrieved 23 October 2013.
109. Wright TC, Stoler MH, Sharma A, Zhang G, Behrens C, Wright TL (2011). "Evaluation of HPV-16 and HPV-18 genotyping for the triage of women with high-risk HPV+ cytology-negative results". Am. J. Clin. Pathol. 136 (4): 578–586. doi:10.1309/ajcptus5exas6dkz. PMID 21917680. Archived from the original on 2013-10-10.
110. Digene HPV HC2 DNA Test Archived 27 August 2010 at the Wayback Machine. Qiagen HPV test
111. "Qiagen to Buy Digene, Maker of Tests for Cancer-Causing Virus". The New York Times. 4 June 2007. Archived from the original on 30 June 2017.
112. "So Close Together for So Long, and Now One". The Washington Post. 20 August 2007. Archived from the original on 6 July 2017.
113. Ronco G (2014). "Efficacy of HPV-based screening for prevention of invasive cervical cancer: follow-up of four European randomised controlled trials". The Lancet. 383: 524–532. doi:10.1016/S0140-6736(13)62218-7.
114. Wentzensen N, von Knebel Doeberitz M (2007). "Biomarkers in cervical cancer screening". Dis. Markers. 23 (4): 315–30. doi:10.1155/2007/678793. PMID 17627065. Archived from the original on 2013-01-28.
115. Molden T, Kraus I, Skomedal H, Nordstrøm T, Karlsen F (June 2007). "PreTect HPV-Proofer: real-time detection and typing of E6/E7 mRNA from carcinogenic human papillomaviruses". J. Virol. Methods. 142 (1–2): 204–12. doi:10.1016/j.jviromet.2007.01.036. PMID 17379322.
116. FDA approval of APTIMA HPV Assay - P100042 Archived 14 December 2012 at the Wayback Machine.
117. Dockter J, Schroder A, Hill C, Guzenski L, Monsonego J, Giachetti C (2009). "Clinical performance of the APTIMA® HPV Assay for the detection of high-risk HPV and high-grade cervical lesions". Journal of Clinical Virology. 45: S55–S61. doi:10.1016/S1386-6532(09)70009-5. PMID 19651370.
118. "Press". gen-probe.com. Archived from the original on 12 December 2012.
119. Dunne EF, Nielson CM, Stone KM, Markowitz LE, Giuliano AR (2006). "Prevalence of HPV Infection among Men: A Systematic Review of the Literature". The Journal of Infectious Diseases. 194 (8): 1044–1057. doi:10.1086/507432. PMID 16991079.
120. Nicolau SM, Camargo CG, Stávale JN, Castelo A, Dôres GB, Lörincz A, de Lima GR (2005). "Human papillomavirus DNA detection in male sexual partners of women with genital human papillomavirus infection". Urology. 65 (2): 251–255. doi:10.1016/j.urology.2004.09.031. PMID 15708032.
121. Aguilar LV, Lazcano-Ponce E, Vaccarella S, Cruz A, Hernández P, Smith JS, Muñoz N, Kornegay JR, Hernández-Avila M, Franceschi S (2006). "Human papillomavirus in men: Comparison of different genital sites". Sexually Transmitted Infections. 82 (1): 31–33. doi:10.1136/sti.2005.015131. PMC 2563819 Freely accessible. PMID 16461598.
122. Weaver BA, Feng Q, Holmes KK, Kiviat N, Lee SK, Meyer C, Stern M, Koutsky LA (2004). "Evaluation of Genital Sites and Sampling Techniques for Detection of Human Papillomavirus DNA in Men". The Journal of Infectious Diseases. 189 (4): 677–685. doi:10.1086/381395. PMID 14767822.
123. Hernandez BY, McDuffie K, Goodman MT, Wilkens LR, Thompson P, Zhu X, Wong W, Ning L (2006). "Comparison of Physician- and Self-Collected Genital Specimens for Detection of Human Papillomavirus in Men". Journal of Clinical Microbiology. 44 (2): 513–517. doi:10.1128/JCM.44.2.513-517.2006. PMC 1392697 Freely accessible. PMID 16455906.
124. Ogilvie GS, Taylor DL, Achen M, Cook D, Krajden M (2008). "Self-collection of genital human papillomavirus specimens in heterosexual men". Sexually Transmitted Infections. 85 (3): 221–225. doi:10.1136/sti.2008.033068. PMID 19066196.
125. Women had similar success in self-sampling, using tampons, swabs, cytobrush and lavage. Petignat P, Faltin DL, Bruchim I, Tramèr MR, Franco EL, Coutlée F (2007). "Are self-collected samples comparable to physician-collected cervical specimens for human papillomavirus DNA testing? A systematic review and meta-analysis". Gynecologic Oncology. 105 (2): 530–535. doi:10.1016/j.ygyno.2007.01.023. PMID 17335880.
126. Partridge JM, Hughes JP, Feng Q, Winer RL, Weaver BA, Xi LF, Stern ME, Lee SK, O'Reilly SF, Hawes SE, Kiviat NB, Koutsky LA (2007). "Genital Human Papillomavirus Infection in Men: Incidence and Risk Factors in a Cohort of University Students". The Journal of Infectious Diseases. 196 (8): 1128–1136. doi:10.1086/521192. PMID 17955430.
127. Burchell AN, Richardson H, Mahmud SM, Trottier H, Tellier PP, Hanley J, Coutlée F, Franco EL (2006). "Modeling the Sexual Transmissibility of Human Papillomavirus Infection using Stochastic Computer Simulation and Empirical Data from a Cohort Study of Young Women in Montreal, Canada". American Journal of Epidemiology. 163 (6): 534–543. doi:10.1093/aje/kwj077. PMID 16421235.
128. Kim JJ (2007). "Vaccine Policy Analyses Can Benefit from Natural History Studies of Human Papillomavirus in Men". The Journal of Infectious Diseases. 196 (8): 1117–1119. doi:10.1086/521199. PMID 17955427.
129. "FAQs for Men". thehpvtest.com. Archived from the original on 5 September 2012.
130. Dunne EF, Nielson CM, Stone KM, Markowitz LE, Giuliano AR (2006). "Prevalence of HPV infection among men: A systematic review of the literature". J. Infect. Dis. 194 (8): 1044–57. doi:10.1086/507432. PMID 16991079.
131. "Human Papillomavirus (HPV) and Men: Questions and Answers". 2007. Archived from the original on 14 September 2008. Retrieved 10 September 2008. Currently, in Canada there is an HPV DNA test approved for women but not for men.
132. "What Men Need to Know About HPV". 2006. Archived from the original on 7 April 2007. Retrieved 4 April 2007. There is currently no FDA-approved test to detect HPV in men. That is because an effective, reliable way to collect a sample of male genital skin cells, which would allow detection of HPV, has yet to be developed.
133. Haedicke, Juliane; Thomas Iftner (2013). "Detection of Immunoglobulin G against E7 of Human Papillomavirus in Non-Small-Cell Lung Cancer". Journal of Oncology. Archived from the original on 18 March 2014. Retrieved 18 March 2014.
134. Rocha-Zavaleta L, Ambrosio JP, Mora-Garcia Mde L, Cruz-Talonia F, Hernandez-Montes J, Weiss-Steider B, Ortiz-Navarrete V, Monroy-Garcia A (2004). "Detection of antibodies against a human papillomavirus (HPV) type 16 peptide that differentiate high-risk from low-risk HPV-associated low-grade squamous intraepithelial lesions" (PDF). Journal of General Virology. 85 (9): 2643–2650. doi:10.1099/vir.0.80077-0. PMID 15302958. Retrieved 18 March 2014.
135. Bolhassani, Azam; Farnaz Zahedifard, Yasaman Taslimi, Mohammad Taghikhani, Bijan Nahavandian, Sima Rafati (2009). "Antibody detection against HPV16 E7 & GP96 fragments as biomarkers in cervical cancer patients" (PDF). Indian J. Med. (130): 533–541. Archived (PDF) from the original on 16 December 2010. Retrieved 18 March 2014.
136. Fitzgerald, Kelly (18 June 2013). "Blood Test May Detect Sexually Transmitted Throat Cancer". Medical News Today. Archived from the original on 7 April 2014. Retrieved 18 March 2014.
137. "Genital Human Papillomavirus (HPV) Infection - Ready-to-Use - Faculty Notes" (PDF). Retrieved 7 February 2018.
138. "FDA approves Gardasil 9 for prevention of certain cancers caused by five additional types of HPV". 10 December 2014. Archived from the original on 10 January 2015. Retrieved 8 March 2015.
139. "Human Papillomavirus Epidemiology and Prevention of Vaccine-Preventable Diseases". CDC.gov. Archived from the original on 3 February 2014. Retrieved 30 January 2014.
140. "Human papillomavirus vaccines. WHO position paper" (PDF). Wkly. Epidemiol. Rec. 84 (15): 118–31. April 2009. PMID 19360985. Archived (PDF) from the original on 24 December 2010.
141. Koliopoulos, George; Nyaga, Victoria N.; Santesso, Nancy; Bryant, Andrew; Martin-Hirsch, Pierre Pl; Mustafa, Reem A.; Schünemann, Holger; Paraskevaidis, Evangelos; Arbyn, Marc (2017-08-10). "Cytology versus HPV testing for cervical cancer screening in the general population". The Cochrane Database of Systematic Reviews. 8: CD008587. doi:10.1002/14651858.CD008587.pub2. ISSN 1469-493X. PMID 28796882.
142. Cite error: The named reference ol2017 was invoked but never defined (see the help page).
143. "CDC recommends only two HPV shots for younger adolescents". CDC. 20 October 2016. Archived from the original on 23 March 2017. Retrieved 24 March 2017.
144. Markowitz LE, Dunne EF, Saraiya M, Lawson HW, Chesson H, Unger ER (March 2007). "Quadrivalent Human Papillomavirus Vaccine: Recommendations of the Advisory Committee on Immunization Practices (ACIP) (Cervical Cancer Screening Among Vaccinated Females)". MMWR Recomm Rep. 56 (RR–2): 1–24 [17]. PMID 17380109. Archived from the original on 20 May 2017.
145. Simon R. M. Dobson; MD; et al. (1 May 2013). "Immunogenicity of 2 Doses of HPV Vaccine in Younger Adolescents vs 3 Doses in Young Women A Randomized Clinical Trial". JAMA. 309 (17): 1793–1802. doi:10.1001/jama.2013.1625. PMID 23632723. Archived from the original on 6 June 2015. Retrieved 2 June 2015.
146. "HPV Vaccine Information For Young Women". CDC. 3 January 2017. Archived from the original on 25 March 2017. Retrieved 24 March 2017.
147. "HPV Virus: Information About Human Papillomavirus". WebMD. Archived from the original on 8 March 2008.
148. "Gardasil patient information leaflet" (PDF). April 2015. Retrieved 2018-07-11.
149. Yvonne Deleré; et al. (September 2014). "The Efficacy and Duration of Vaccine Protection Against Human Papillomavirus: A Systematic Review and Meta-analysis". Dtsch Arztebl Int. 111: 35–36. doi:10.3238/arztebl.2014.0584. PMC 4174682 Freely accessible. PMID 25249360.
150. "FDA approves Gardasil 9 for prevention of certain cancers caused by five additional types of HPV" (press release). 10 December 2014. Archived from the original on 10 January 2015. Retrieved 28 February 2015.
151. "CDC — Condom Effectiveness — Male Latex Condoms and Sexually Transmitted Diseases". Centers for Disease Control and Prevention (CDC). 22 October 2009. Archived from the original on 17 October 2009. Retrieved 23 October 2009.
152. "Information About What is Human Papillomavirus (HPV)?". City of Toronto Public Health Agency. September 2010. Retrieved 20 July 2011.[permanent dead link]
153. "Human papillomavirus - Public Health Agency of Canada". phac-aspc.gc.ca. Archived from the original on 23 August 2015.
154. "Genital HPV Infection Fact Sheet". Centers for Disease Control and Prevention (CDC). 10 April 2008. Archived from the original on 11 September 2012. Retrieved 13 November 2009.
155. "HPV Vaccine Information For Young Women". Centers for Disease Control and Prevention (CDC). 26 June 2008. Archived from the original on 26 October 2009. Retrieved 13 November 2009.
156. American Cancer Society. "What Are the Risk Factors for Cervical Cancer?". Archived from the original on 19 February 2008. Retrieved 21 February 2008.
157. "Cure for HPV". Webmd.com. Archived from the original on 18 August 2010. Retrieved 29 August 2010.
158. Gilbert LK, Alexander L, Grosshans JF, Jolley L (2003). "Answering frequently asked questions about HPV". Sex. Transm. Dis. 30 (3): 193–4. doi:10.1097/00007435-200303000-00002. PMID 12616133. Archived from the original on 24 December 2011.
159. "Updated U.S. Public Health Service guidelines for the management of occupational exposures to HIV and recommendations for postexposure prophylaxis." Centers for Disease Control and Prevention. Archived from the original on 16 November 2015. Retrieved 23 October 2015.
160. Desai, Monica; Woodhall, Sarah C; Nardone, Anthony; Burns, Fiona; Mercey, Danielle; Gilson, Richard (2015). "Active recall to increase HIV and STI testing: a systematic review". Sexually Transmitted Infections: sextrans–2014–051930. doi:10.1136/sextrans-2014-051930. ISSN 1368-4973.
161. "Human papillomavirus vaccines: WHO position paper, October 2014" (PDF). Weekly Epidemiological Record. 89: 465–492. 24 October 2014. PMID 25346960. Archived (PDF) from the original on 19 October 2015.
162. Gavillon N, Vervaet H, Derniaux E, Terrosi P, Graesslin O, Quereux C (2010). "Papillomavirus humain (HPV) : comment ai-je attrapé ça ?". Gynécologie Obstétrique & Fertilité. 38 (3): 199–204. doi:10.1016/j.gyobfe.2010.01.003. PMID 20189438.
163. Dunne EF, Unger ER, Sternberg M, McQuillan G, Swan DC, Patel SS, Markowitz LE (February 2007). "Prevalence of HPV infection among females in the United States". JAMA. 297 (8): 813–9. doi:10.1001/jama.297.8.813. PMID 17327523. Archived from the original on 30 May 2011.
164. "American Social Health Association — HPV Resource Center". Archived from the original on 18 July 2007. Retrieved 17 August 2007.
165. "American Social Health Association — National HPV and Cervical Cancer Prevention Resource Center". Archived from the original on 19 June 2008. Retrieved 1 July 2008.
166. "HPV vaccine report", STD, HIV, Planned Parenthood, In fact, the lifetime risk for contracting HPV is at least 50 percent for all sexually active women and men, and, it is estimated that, by the age of 50, at least 80 percent of women will have acquired sexually transmitted HPV (CDC, 2004; CDC, 2006).
167. Weinstock H, Berman S, Cates W (January–February 2004). "Sexually Transmitted Diseases Among American Youth: Incidence and Prevalence Estimates, 2000". Perspectives on Sexual and Reproductive Health. Gutt Macher. 36 (1): 6–10. doi:10.1363/3600604. PMID 14982671. Archived from the original on 4 July 2008.
168. Koutsky, LA (1997). "Epidemiology of human papilomavirus infection". The American Journal of Medicine. 102: 3–8. doi:10.1016/s0002-9343(97)00177-0.
169. Revzina NV, Diclemente RJ (2005). "Prevalence and incidence of human papillomavirus infection in women in the USA: a systematic review". International Journal of STD & AIDS. 16 (8): 528–37. doi:10.1258/0956462054679214. PMID 16105186. The prevalence of HPV reported in the assessed studies ranged from 14% to more than 90%.
170. McCullough, Marie (28 February 2007). "Cancer-virus strains rarer than first estimated". The Philadelphia Inquirer. Archived from the original on 10 March 2007. Retrieved 2 March 2007.
171. Brown, David (28 February 2007) [The Washington Post, "More American Women Have HPV Than Previously Thought"]. "Study finds more women than expected have HPV". San Francisco Chronicle. Archived from the original on 9 November 2007. Retrieved 2 March 2007.
172. Tanner, Lindsey (11 March 2008). "Study Finds 1 in 4 US Teens Has a STD". Newsvine. Associated Press. Archived from the original on 16 March 2008. Retrieved 17 March 2008.
173. "MMWR: Summary of Notifiable Diseases". Morbidity and Mortality Weekly Report. CDC. Archived from the original on 17 August 2014. Retrieved 18 August 2014.
174. Reportable diseases Archived 12 April 2016 at the Wayback Machine., from MedlinePlus, a service of the U.S. National Library of Medicine, from the National Institutes of Health. Update: 19 May 2013 by Jatin M. Vyas. Also reviewed by David Zieve.
175. Human papillomaviruses. World Health Organization, International Agency for Research on Cancer. 2007. ISBN 978-92-832-1290-4.
176. "HPV — the Shy Virus" (radio program). Sound print. 6 December 2008. Archived from the original on 28 March 2009. Retrieved 6 December 2008.
177. Picken RN, Yang HL (1987). "The integration of HPV-18 into HeLa cells has involved duplication of part of the viral genome as well as human DNA flanking sequences". Nucleic Acids Research. 15 (23): 10068. doi:10.1093/nar/15.23.10068. PMC 306572 Freely accessible. PMID 2827110.
178. Lipke, MM (December 2006). "An armamentarium of wart treatments". Clinical medicine & research. 4 (4): 273–93. PMID 17210977. |